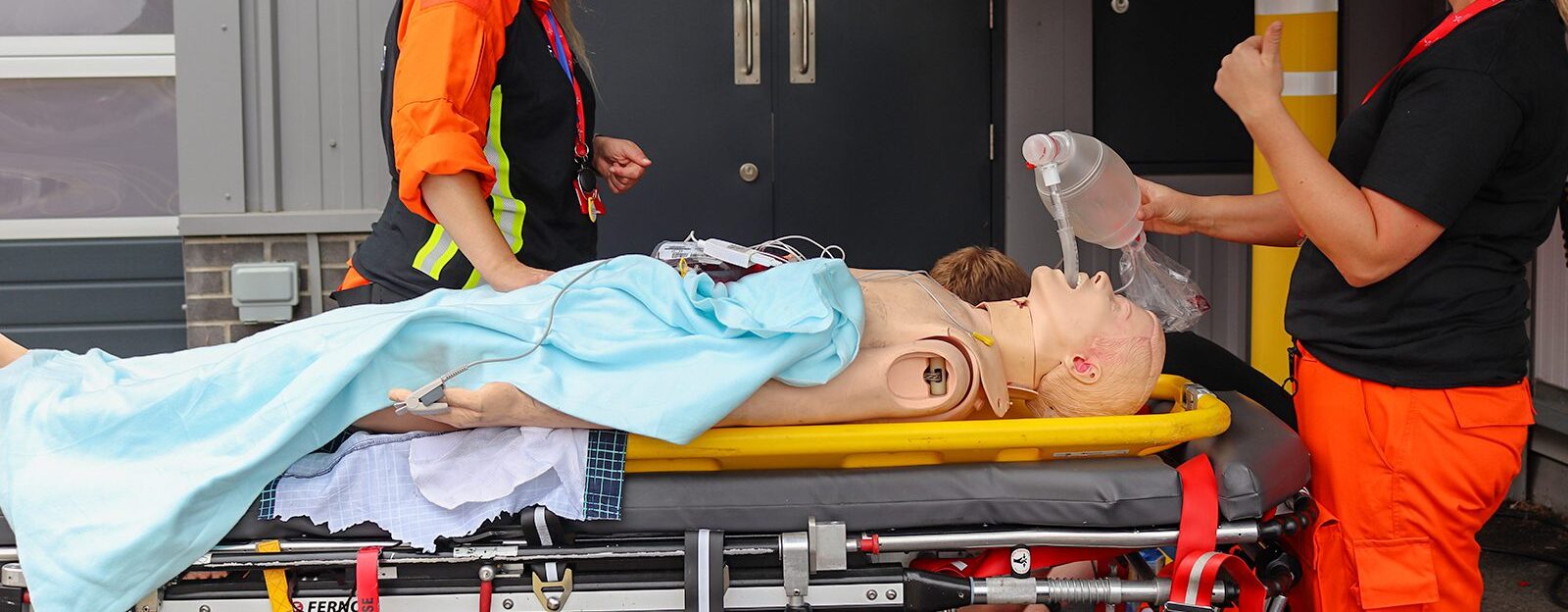
When someone is seriously ill or injured, every second matters. Our doctors and critical care paramedics bring lifesaving hospital-level care directly to the patient - whether they’re at home, on the roadside, or anywhere in between.
From giving blood transfusions and advanced pain relief to providing sedation, and even performing surgical procedures at the scene, our crews can start urgent treatment before transferring our patients to the most appropriate hospital for their ongoing care – and it’s all possible thanks to the generosity of incredible people like you.
One of the advanced procedures our teams can carry out is giving critically unwell and injured people a pre-hospital emergency anaesthetic and, in this article, we take a look into a procedure which can make a lifesaving difference to the people we’re called to help.
When is a pre-hospital emergency anaesthetic needed?
A pre-hospital emergency anaesthetic is given in certain medical emergencies, such as a severe head injury, or a major injury to the chest which has compromised the patient’s breathing. It enables us to take over a patient’s breathing to protect their airway or their brain by controlling oxygenation and ventilation.
This involves administering pain relief, strong sedation so we can gently place a breathing tube into the patient’s trachea (windpipe).
How we carry out the procedure
We have standard operating procedures to support our decision making in identifying the patients who could benefit from a pre-hospital anaesthetic before they are transferred to hospital.
We use checklists to ensure that we have all the equipment we need and can conduct the procedure as safely as possible, before checking all parameters are optimised before starting the procedure. Together, the team talks through potential challenges and agrees on the plan – and the backup plan. This two-person approach ensures calm, clear decision making, even in the most pressured situations.
Our crews train extensively to make this process swift, smooth and safe. Everyone is encouraged to speak up, share what they see and help secure the best possible outcome for the patient.
The right equipment at the right time
Once a pre-hospital emergency anaesthetic has been administered, strong medications enable us to place a breathing tube into the trachea to the lungs which is then connected to a ventilator. This allows us to carefully control how much oxygen the patient receives and monitor the carbon dioxide they breathe out.
Your support means our crews have the correct, special equipment they need to do this. This includes:
- Direct Laryngoscope: A curved blade with a light that helps us follow the tongue, pass the epiglottis to find the vocal cords – our route into the trachea.
- Video Laryngoscope: A similar tool, but with a tiny camera and screen, allowing us to see the airway without needing a direct line of sight.
Once we can clearly see the trachea, we use a thin, flexible introducer called a bougie. The breathing tube slides over the bougie and into place. Then we inflate a small balloon at the bottom of the tube to create a secure seal. This breathing tube is then connected to a mechanical ventilator, which carefully controls the delivery of oxygen to the patient.
It’s a highly complex and advanced procedure that our crews regularly train for and simulate for both adult and paediatric patients. We also carry our equipment in different sizes, ensuring that we can perform the procedure on even the youngest and smallest of patients.
It’s all thanks to you
We care deeply about the work we do and the people we help. The equipment carried by our helicopters and critical care cars enables enhanced care, including pre-hospital emergency anaesthetics, at the incident scene – when the patient needs it most. We’re fuelled entirely by donations, without any regular government funding, so your support powers every single tasking, every procedure, and every second chance.